Medical Device Assembly: Better One of Better Two?
Cataracts, glaucoma, macular degeneration, presbyopia, diabetic retinopathy, posterior uveitis and other vision-related conditions make ophthalmology one of the most dynamic market segments in the medical device industry. An aging population, proposed federal healthcare reform and an increasing number of elective surgeries is creating a huge demand for diagnostic instruments, surgical equipment, lasers, intraocular lens implants, shunts, artificial retinas and other products.

As most people age, they become wiser. But, gradual vision loss is something that even the smartest people in the world can’t avoid. That simple fact of life is good news for the ophthalmic device industry.
Cataracts, glaucoma, macular degeneration, presbyopia, diabetic retinopathy, posterior uveitis and other vision-related conditions make ophthalmology one of the most dynamic market segments in the medical device industry. An aging population, proposed federal healthcare reform and an increasing number of elective surgeries, such as Lasik treatment, is creating a huge demand for diagnostic instruments, surgical equipment, lasers, intraocular lens implants, shunts, artificial retinas and other products.
Approximately 50 percent of all adults in the United States don’t have 20/20 vision, because they are nearsighted, farsighted or have an astigmatism, which is an irregular curve of the cornea. By 2020, the number of people who are blind or have low vision is projected to increase dramatically.
“Blindness or low vision affects 3.3 million Americans age 40 or over . . . and this figure [will] reach 5.5 million by the year 2020,” says Elias Zerhouni, M.D., director of the National Institutes of Health (Bethesda, MD), which operates the Eye Disease Prevalence Research Group and the National Eye Institute. “As our population lives longer, eye disease will be an ever greater concern. Low vision and blindness increase significantly with age, particularly in people over age 65.”
A recent study conducted by RTI International (Research Triangle Park, NC) and the Centers for Disease Control and Prevention (Atlanta) predicts there will be a huge demand for ophthalmic devices over the next four decades. “The aging U.S. population will lead to a large increase in early and advanced age-related macular degeneration,” claims David Rein, a senior research economist at RTI.
“By 2050, the number of people with early age-related macular degeneration will double to more than 17.8 million,” Rein points out. At the same time, he expects the number of cases of diabetic retinopathy, which is the leading cause of blindness among working-age adults in the United States, to increase from 5.5 million to 16 million.
“The good news is that medical technologies are changing rapidly,” says Rein. “Ten years ago, there were no treatments for age-related macular degeneration. With luck, tomorrow’s discoveries will lead to far greater reductions in visual impairment and blindness.”
According to MedMarket Diligence LLC (Foothill Ranch, CA), the worldwide ophthalmic products market exceeds $22 billion and is growing at more than 10 percent annually. The industry is dominated by several major players, such as Abbott Medical Optics Inc. (Santa Ana, CA), Alcon Laboratories Inc. (Fort Worth, TX), Bausch & Lomb Inc. (Rochester, NY) and Carl Zeiss Meditec AG (Jena, Germany). However, numerous small start-up companies specialize in niche segments, such as cataract, corneal or refractive surgery.
No matter the size of the company, ophthalmic manufacturers are focusing their efforts on making surgical procedures faster, easier, more accurate and more affordable. There’s also a growing trend toward drug-device combination products.
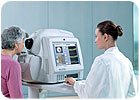
Ophthalmologists are always looking for equipment that makes them better clinicians. They want instruments that provide information that allows them to make better diagnoses and more efficient treatment decisions in a patient-friendly manner.
“The latest trend is toward noninvasive diagnostic imaging,” says Andrew Shatz, M.D., an ophthalmologist at the Woolfson Eye Institute (Atlanta). “High-speed ultrasound and scanning laser tomography are both giving increasingly sharper resolution of the microscopic structures of the eye, allowing for a more detailed view of pathology.
“This has also allowed us to visualize the relationship between the different regions of the eye in a way we have never been able to before, without having to resort to intravenous dye injection,” explains Shatz. “More doctors are adopting technology that allows us to image the back of the eye without the need for dilation.”
“We now have incredibly precise imaging devices called OCT (optical coherence tomography) that allow us to create microscopic images of structures inside the eye that were never before visible,” adds John Hovanesian, M.D., an ophthalmologist at Harvard Eye Associates (Laguna Hills, CA) and a clinical instructor at UCLA’s Jules Stein Eye Institute (Los Angeles). “This greatly aids in diagnosis of conditions like diabetic eye problems, eye tumors and macular degeneration.”
An OCT allows an ophthalmologist to construct three-dimensional images of living eye tissue with better resolution than a traditional MRI scan. Better yet, the procedure can be performed in a doctor’s office instead of a hospital.
Today’s new breed of diagnostic instruments use state-of-the-art technology to objectively measure and quantify vision disorders. For instance, engineers at Optos Inc. (Marlborough, MA) recently developed a new type of imaging device that provides an ultra-widefield view of the retina. It allows ophthalmologists to see more than 80 percent of the retina, compared to a traditional camera that provides a much narrower view-about 11 percent. The device uses scanning coherent laser light rather than full spectrum white light that’s typically used by cameras and other forms of ophthalmoscopy.
Researchers at the National Eye Institute (Bethesda, MD) and the National Aeronautics and Space Administration (NASA, Washington, DC) recently adapted a compact fiber-optic probe developed for the space program into the world’s first noninvasive early detection device for cataracts, the leading cause of vision loss worldwide. The new device is based on a laser light technique called dynamic light scattering (DLS).
It was initially developed to analyze the growth of protein crystals in a zero-gravity space environment. The tabletop DLS device is used to detect the earliest damage to lens proteins, triggering an early warning for cataract formation and blindness.
“Much of the work [in the diagnostic instrument field] is going into finding ways to treat presbyopia to enable people to get rid of their reading glasses,” says James Ohneck, CEO of Oculatek Inc. (Cleveland). The start-up company has developed a transscleral light therapy system that uses a low level of infrared light at a specific wavelength. “It helps strengthen the ciliary muscle, which weakens as the eye ages and is one of the factors that leads to the eye’s inability to accommodate,” Ohneck points out.
“It is therapy, not surgery,” adds Ohneck. “The patient has several short therapy sessions where they look into a binocular while the eye is dosed with infrared light. The treatment does not harm the eye and there is no pain associated with the procedure. It’s unique because it is the first device of its kind to therapeutically treat presbyopia without an invasive surgical procedure. Newer technologies being developed involve implanting special lenses through a surgical procedure or modifying the shape of the eye to adjust vision.”
Even noninvasive ophthalmic procedures must be cleared by the U.S. Food and Drug Administration (FDA, Washington, DC), which often hinders start-up manufacturers and prevents them from quickly ramping up production. For instance, Oculatek’s device is still undergoing trials with the FDA. If approved, it won’t be readily available to ophthalmologists for several more years.
“The challenges around new devices are regulatory in nature, such as getting FDA approval and validating the efficacy through clinical trials,” says Ohneck, who holds a degree in electronic engineering. “This takes time and money. Investors are reluctant to put money into products that don’t have the trials, so it’s a chicken and egg; you need money to do clinicals, but you can’t get it until the clinicals are completed.”
To reduce costs, many start-up manufacturers outsource assembly to third parties. For instance, Oculatek is working with Valtronic Technologies Inc. (Solon, OH). That allows Ohneck and his colleagues to focus their attention on product development.
Ophthalmic devices are typically assembled in clean rooms. Large manufacturers, such as Alcon, have recently been focusing their efforts on ergonomics and automation. Alcon’s Fort Worth plant recently celebrated its 50 anniversary, and the company is currently building a new facility in Singapore to supply the fast-growing Asian market.
“In our more manual assembly areas, we have invested in adjustable workstations and eliminated microscopes to make our operators more comfortable,” says Melissa Mota, a company spokesperson. “In addition, we have invested heavily to automate mid- and higher-volume operations and products. Our focus has been on advancing our assembly processes to be flexi-ble with high-mix automation, in order to satisfy increasing demand for our products.”

“The new revolution is almost at hand,” claims Shatz. “Improved lens and cataract surgery technology, in combination with the baby-boomer generation now developing cataracts, has created the perfect breeding ground for presbyopic lens implants. This technology will overtake laser vision correction as the primary means of correcting vision in the next five to 10 years.”
Intraocular lenses (IOLs) are typically made of either acrylic or silicone. Early versions were made of an acrylic polymer called PMMA, which is what led to the discovery of using IOLs in cataract surgery.
The latest trend in IOLs is toward corrective, foldable lenses that are structurally designed to minimize secondary cataracts from occurring. Most companies developing intraocular implants are focusing their efforts on devices that treat back-of-the-eye diseases, such as glaucoma and acute macular degeneration.
For instance, Alcon recently unveiled the third generation of its Restor lens. The multi-focal device contains 12 concentric “steps” around the optic zone of the lens, which appear as rings. They create different focusing levels from near to distant vision. The surgical procedure is painless and only takes about 20 minutes. Some ophthalmologists are recommending the procedure as an alternative to the more controversial Lasik treatment.
In addition, engineers and doctors are currently developing polymeric drug delivery devices that are implanted at the time of cataract surgery along with an IOL. The hybrid devices are designed to treat the most common postoperative complications, such as inflammation, infection and secondary cataracts.
“Drug therapy ease of use is of considerable importance as the world’s population continues to age,” says Tracy Klein, CEO of Inson Medical Systems Inc. (Bellevue, WA). “There is a considerable opportunity to reformulate older pharmaceuticals into implantable devices. Eye drops are the standard of care for most ophthalmic diseases, yet they have poor penetration into the eye and are inconvenient for patients to administer, often with four to six times per day dosing.”
Klein’s company is developing front-of-the-eye drug delivery beads that are smaller than a grain of rice. “We plan to utilize this expertise on future products for back-of-the-eye applications,” he explains. “We are also in very early development discussions with potential partners who are interested in utilizing our technology to create IOLs capable of drug delivery.”
Implantable intraocular lenses pose numerous manufacturing challenges. “The main challenge for us is to make a device small enough to be inserted with the lens, yet big enough to hold enough drug,” says Klein. “There are also technical challenges to overcome with existing injection molding techniques when making devices this small.”
For instance, lenses must be extremely thin to be flexible and comfortable to patients. Klein believes the ophthalmic device industry may be able to adapt existing semiconductor manufacturing technology and equipment if devices get smaller.
“[However], ophthalmic implantable devices must be as long-acting as possible for obvious reasons,” says Klein. “Therefore, they are unlikely to get much smaller. In addition, surgeons generally want devices they can retrieve if necessary.”
“The goal at the moment is to achieve better efficacy with less invasive procedures,” notes Paul Ashton, M.D., president of pSivida Corp. (Watertown, MA). “There are a lot of blinding diseases for which there are no drug treatments yet approved. These diseases include dry age-related macular degeneration (AMD) and diabetic retinopathy.
“Recently, there have been some drug treatments approved for wet-form AMD, but this typically consists of an injection into the eye every couple of months,” Ashton points out. “A [more] effective and less invasive treatment for this disease [would] be quite an advantage.”
Ashton and his colleagues have recently developed a variety of ophthalmic devices for either implantation or injection into the eye. The devices are made from a proprietary porous silicon material.
Vitrasert was the first sustained release device approved for back-of-the-eye applications. It’s about the size of a pepper corn (6 millimeters long and 2.5 millimeters wide). The device is surgically implanted into the eye, where it releases drugs for six to eight months. “Because the drug is released directly into the eye, it requires approximately 20,000 times less drug than would be needed if given intravenously,” says Ashton.
Retisert is a smaller device that is 5.25 millimeters long and 1.5 millimeters wide, or about the size of a grain of rice. It lasts 2.5 years after implantation into the eye. “As it releases its drug directly into the eye, it delivers about 200,000 times less drug than would be needed if the patient took the drug orally,” claims Ashton. It is the only FDA-approved treatment for posterior uveitis, a potentially blinding disease. “Implanting either Vitrasert or Retisert is a little like having a cataract operation,” says Ashton.
The next step in the evolution of this series of implantable devices is called Iluvien. The device is much smaller than Retisert (only 3 millimeters long and 0.5 millimeter wide), but it’s designed to last about the same length of time. “It’s about the length of an eyelash and is small enough to fit into a needle,” says Ashton. “This allows it to be injected directly into the eye in an office visit [as opposed to outpatient surgery, with fewer complications]. The procedure is also far cheaper.”
According to Ashton, future ophthalmic devices will continue to get smaller and more sophisticated. “Bioerodible systems are already in early stages of testing,” he points out. “Applying existing semiconductor [manufacturing processes] and nanotechnology [will create] ‘intelligent’ devices that respond to a disease or tell a physician if they are about to run out [of a drug].”
In addition to improved lens implants and drug-device hybrids, another new device that intrigues many ophthalmologists is the artificial retina. “This device has given hope to patients who have lost vision from disabling retinal diseases such as macular degeneration,” says Shatz. “While the resolution is currently only able to allow for ambulatory vision, higher resolution electrode arrays under development will be able to differentiate letters and objects.”
The artificial retina, called Argus II, is being developed by engineers at five U.S. Department of Energy laboratories and four universities. It consists of an array of 60 electrodes that are attached to the retina. The electrodes conduct information acquired from an external camera to the retina to provide a rudimentary form of sight. The device has already been implanted in six patients. A newer, higher resolution model will be available within the next few years.
To learn more about the device, see "The 'Holy Grail' of Ophthalmic Devices" at www.assemblymag.com

As most people age, they become wiser. But, gradual vision loss is something that even the smartest people in the world can’t avoid. That simple fact of life is good news for the ophthalmic device industry.
Cataracts, glaucoma, macular degeneration, presbyopia, diabetic retinopathy, posterior uveitis and other vision-related conditions make ophthalmology one of the most dynamic market segments in the medical device industry. An aging population, proposed federal healthcare reform and an increasing number of elective surgeries, such as Lasik treatment, is creating a huge demand for diagnostic instruments, surgical equipment, lasers, intraocular lens implants, shunts, artificial retinas and other products.
Approximately 50 percent of all adults in the United States don’t have 20/20 vision, because they are nearsighted, farsighted or have an astigmatism, which is an irregular curve of the cornea. By 2020, the number of people who are blind or have low vision is projected to increase dramatically.
“Blindness or low vision affects 3.3 million Americans age 40 or over . . . and this figure [will] reach 5.5 million by the year 2020,” says Elias Zerhouni, M.D., director of the National Institutes of Health (Bethesda, MD), which operates the Eye Disease Prevalence Research Group and the National Eye Institute. “As our population lives longer, eye disease will be an ever greater concern. Low vision and blindness increase significantly with age, particularly in people over age 65.”
A recent study conducted by RTI International (Research Triangle Park, NC) and the Centers for Disease Control and Prevention (Atlanta) predicts there will be a huge demand for ophthalmic devices over the next four decades. “The aging U.S. population will lead to a large increase in early and advanced age-related macular degeneration,” claims David Rein, a senior research economist at RTI.
“By 2050, the number of people with early age-related macular degeneration will double to more than 17.8 million,” Rein points out. At the same time, he expects the number of cases of diabetic retinopathy, which is the leading cause of blindness among working-age adults in the United States, to increase from 5.5 million to 16 million.
“The good news is that medical technologies are changing rapidly,” says Rein. “Ten years ago, there were no treatments for age-related macular degeneration. With luck, tomorrow’s discoveries will lead to far greater reductions in visual impairment and blindness.”
According to MedMarket Diligence LLC (Foothill Ranch, CA), the worldwide ophthalmic products market exceeds $22 billion and is growing at more than 10 percent annually. The industry is dominated by several major players, such as Abbott Medical Optics Inc. (Santa Ana, CA), Alcon Laboratories Inc. (Fort Worth, TX), Bausch & Lomb Inc. (Rochester, NY) and Carl Zeiss Meditec AG (Jena, Germany). However, numerous small start-up companies specialize in niche segments, such as cataract, corneal or refractive surgery.
No matter the size of the company, ophthalmic manufacturers are focusing their efforts on making surgical procedures faster, easier, more accurate and more affordable. There’s also a growing trend toward drug-device combination products.

An OCT allows ophthalmologists to construct three-dimensional images of living eye tissue with better resolution than a traditional MRI scan.
Diagnostic Tools
Traditionally, the ophthalmic industry is divided into two main segments: diagnostic instruments and surgical devices. Diagnostic instruments are used by ophthalmologists to examine their patients. They include refractors (the “better-one, better-two” device that’s used in conjunction with an eye chart), slit lamps (an upright microscope equipped with a bright light) and tonometers (a device that measures eye pressure).Ophthalmologists are always looking for equipment that makes them better clinicians. They want instruments that provide information that allows them to make better diagnoses and more efficient treatment decisions in a patient-friendly manner.
“The latest trend is toward noninvasive diagnostic imaging,” says Andrew Shatz, M.D., an ophthalmologist at the Woolfson Eye Institute (Atlanta). “High-speed ultrasound and scanning laser tomography are both giving increasingly sharper resolution of the microscopic structures of the eye, allowing for a more detailed view of pathology.
“This has also allowed us to visualize the relationship between the different regions of the eye in a way we have never been able to before, without having to resort to intravenous dye injection,” explains Shatz. “More doctors are adopting technology that allows us to image the back of the eye without the need for dilation.”
“We now have incredibly precise imaging devices called OCT (optical coherence tomography) that allow us to create microscopic images of structures inside the eye that were never before visible,” adds John Hovanesian, M.D., an ophthalmologist at Harvard Eye Associates (Laguna Hills, CA) and a clinical instructor at UCLA’s Jules Stein Eye Institute (Los Angeles). “This greatly aids in diagnosis of conditions like diabetic eye problems, eye tumors and macular degeneration.”
An OCT allows an ophthalmologist to construct three-dimensional images of living eye tissue with better resolution than a traditional MRI scan. Better yet, the procedure can be performed in a doctor’s office instead of a hospital.
Today’s new breed of diagnostic instruments use state-of-the-art technology to objectively measure and quantify vision disorders. For instance, engineers at Optos Inc. (Marlborough, MA) recently developed a new type of imaging device that provides an ultra-widefield view of the retina. It allows ophthalmologists to see more than 80 percent of the retina, compared to a traditional camera that provides a much narrower view-about 11 percent. The device uses scanning coherent laser light rather than full spectrum white light that’s typically used by cameras and other forms of ophthalmoscopy.
Researchers at the National Eye Institute (Bethesda, MD) and the National Aeronautics and Space Administration (NASA, Washington, DC) recently adapted a compact fiber-optic probe developed for the space program into the world’s first noninvasive early detection device for cataracts, the leading cause of vision loss worldwide. The new device is based on a laser light technique called dynamic light scattering (DLS).
It was initially developed to analyze the growth of protein crystals in a zero-gravity space environment. The tabletop DLS device is used to detect the earliest damage to lens proteins, triggering an early warning for cataract formation and blindness.
“Much of the work [in the diagnostic instrument field] is going into finding ways to treat presbyopia to enable people to get rid of their reading glasses,” says James Ohneck, CEO of Oculatek Inc. (Cleveland). The start-up company has developed a transscleral light therapy system that uses a low level of infrared light at a specific wavelength. “It helps strengthen the ciliary muscle, which weakens as the eye ages and is one of the factors that leads to the eye’s inability to accommodate,” Ohneck points out.
“It is therapy, not surgery,” adds Ohneck. “The patient has several short therapy sessions where they look into a binocular while the eye is dosed with infrared light. The treatment does not harm the eye and there is no pain associated with the procedure. It’s unique because it is the first device of its kind to therapeutically treat presbyopia without an invasive surgical procedure. Newer technologies being developed involve implanting special lenses through a surgical procedure or modifying the shape of the eye to adjust vision.”
Even noninvasive ophthalmic procedures must be cleared by the U.S. Food and Drug Administration (FDA, Washington, DC), which often hinders start-up manufacturers and prevents them from quickly ramping up production. For instance, Oculatek’s device is still undergoing trials with the FDA. If approved, it won’t be readily available to ophthalmologists for several more years.
“The challenges around new devices are regulatory in nature, such as getting FDA approval and validating the efficacy through clinical trials,” says Ohneck, who holds a degree in electronic engineering. “This takes time and money. Investors are reluctant to put money into products that don’t have the trials, so it’s a chicken and egg; you need money to do clinicals, but you can’t get it until the clinicals are completed.”
To reduce costs, many start-up manufacturers outsource assembly to third parties. For instance, Oculatek is working with Valtronic Technologies Inc. (Solon, OH). That allows Ohneck and his colleagues to focus their attention on product development.
Ophthalmic devices are typically assembled in clean rooms. Large manufacturers, such as Alcon, have recently been focusing their efforts on ergonomics and automation. Alcon’s Fort Worth plant recently celebrated its 50 anniversary, and the company is currently building a new facility in Singapore to supply the fast-growing Asian market.
“In our more manual assembly areas, we have invested in adjustable workstations and eliminated microscopes to make our operators more comfortable,” says Melissa Mota, a company spokesperson. “In addition, we have invested heavily to automate mid- and higher-volume operations and products. Our focus has been on advancing our assembly processes to be flexi-ble with high-mix automation, in order to satisfy increasing demand for our products.”

This telescopic implant is 4 millimeters long and contains two wide-angle glass lenses. It is designed to treat age-related macular degeneration.
Implantable Devices
One of newest technological advances on the surgical side of the ophthalmic device industry is the correction of presbyopia, which affects 90 million people in the United States, with multifocal and accommodating implants. “These not only improve distance vision without glasses, but also decrease the need for readers,” says Shatz. “This market has been heating up over the last few years. What has started out with three competing lens models will [eventually] blossom to 10 or more different technologies, all aimed at achieving the holy grail of ophthalmology.“The new revolution is almost at hand,” claims Shatz. “Improved lens and cataract surgery technology, in combination with the baby-boomer generation now developing cataracts, has created the perfect breeding ground for presbyopic lens implants. This technology will overtake laser vision correction as the primary means of correcting vision in the next five to 10 years.”
Intraocular lenses (IOLs) are typically made of either acrylic or silicone. Early versions were made of an acrylic polymer called PMMA, which is what led to the discovery of using IOLs in cataract surgery.
The latest trend in IOLs is toward corrective, foldable lenses that are structurally designed to minimize secondary cataracts from occurring. Most companies developing intraocular implants are focusing their efforts on devices that treat back-of-the-eye diseases, such as glaucoma and acute macular degeneration.
For instance, Alcon recently unveiled the third generation of its Restor lens. The multi-focal device contains 12 concentric “steps” around the optic zone of the lens, which appear as rings. They create different focusing levels from near to distant vision. The surgical procedure is painless and only takes about 20 minutes. Some ophthalmologists are recommending the procedure as an alternative to the more controversial Lasik treatment.
In addition, engineers and doctors are currently developing polymeric drug delivery devices that are implanted at the time of cataract surgery along with an IOL. The hybrid devices are designed to treat the most common postoperative complications, such as inflammation, infection and secondary cataracts.
“Drug therapy ease of use is of considerable importance as the world’s population continues to age,” says Tracy Klein, CEO of Inson Medical Systems Inc. (Bellevue, WA). “There is a considerable opportunity to reformulate older pharmaceuticals into implantable devices. Eye drops are the standard of care for most ophthalmic diseases, yet they have poor penetration into the eye and are inconvenient for patients to administer, often with four to six times per day dosing.”
Klein’s company is developing front-of-the-eye drug delivery beads that are smaller than a grain of rice. “We plan to utilize this expertise on future products for back-of-the-eye applications,” he explains. “We are also in very early development discussions with potential partners who are interested in utilizing our technology to create IOLs capable of drug delivery.”
Implantable intraocular lenses pose numerous manufacturing challenges. “The main challenge for us is to make a device small enough to be inserted with the lens, yet big enough to hold enough drug,” says Klein. “There are also technical challenges to overcome with existing injection molding techniques when making devices this small.”
For instance, lenses must be extremely thin to be flexible and comfortable to patients. Klein believes the ophthalmic device industry may be able to adapt existing semiconductor manufacturing technology and equipment if devices get smaller.
“[However], ophthalmic implantable devices must be as long-acting as possible for obvious reasons,” says Klein. “Therefore, they are unlikely to get much smaller. In addition, surgeons generally want devices they can retrieve if necessary.”
“The goal at the moment is to achieve better efficacy with less invasive procedures,” notes Paul Ashton, M.D., president of pSivida Corp. (Watertown, MA). “There are a lot of blinding diseases for which there are no drug treatments yet approved. These diseases include dry age-related macular degeneration (AMD) and diabetic retinopathy.
“Recently, there have been some drug treatments approved for wet-form AMD, but this typically consists of an injection into the eye every couple of months,” Ashton points out. “A [more] effective and less invasive treatment for this disease [would] be quite an advantage.”
Ashton and his colleagues have recently developed a variety of ophthalmic devices for either implantation or injection into the eye. The devices are made from a proprietary porous silicon material.
Vitrasert was the first sustained release device approved for back-of-the-eye applications. It’s about the size of a pepper corn (6 millimeters long and 2.5 millimeters wide). The device is surgically implanted into the eye, where it releases drugs for six to eight months. “Because the drug is released directly into the eye, it requires approximately 20,000 times less drug than would be needed if given intravenously,” says Ashton.
Retisert is a smaller device that is 5.25 millimeters long and 1.5 millimeters wide, or about the size of a grain of rice. It lasts 2.5 years after implantation into the eye. “As it releases its drug directly into the eye, it delivers about 200,000 times less drug than would be needed if the patient took the drug orally,” claims Ashton. It is the only FDA-approved treatment for posterior uveitis, a potentially blinding disease. “Implanting either Vitrasert or Retisert is a little like having a cataract operation,” says Ashton.
The next step in the evolution of this series of implantable devices is called Iluvien. The device is much smaller than Retisert (only 3 millimeters long and 0.5 millimeter wide), but it’s designed to last about the same length of time. “It’s about the length of an eyelash and is small enough to fit into a needle,” says Ashton. “This allows it to be injected directly into the eye in an office visit [as opposed to outpatient surgery, with fewer complications]. The procedure is also far cheaper.”
According to Ashton, future ophthalmic devices will continue to get smaller and more sophisticated. “Bioerodible systems are already in early stages of testing,” he points out. “Applying existing semiconductor [manufacturing processes] and nanotechnology [will create] ‘intelligent’ devices that respond to a disease or tell a physician if they are about to run out [of a drug].”
In addition to improved lens implants and drug-device hybrids, another new device that intrigues many ophthalmologists is the artificial retina. “This device has given hope to patients who have lost vision from disabling retinal diseases such as macular degeneration,” says Shatz. “While the resolution is currently only able to allow for ambulatory vision, higher resolution electrode arrays under development will be able to differentiate letters and objects.”
The artificial retina, called Argus II, is being developed by engineers at five U.S. Department of Energy laboratories and four universities. It consists of an array of 60 electrodes that are attached to the retina. The electrodes conduct information acquired from an external camera to the retina to provide a rudimentary form of sight. The device has already been implanted in six patients. A newer, higher resolution model will be available within the next few years.
To learn more about the device, see "The 'Holy Grail' of Ophthalmic Devices" at www.assemblymag.com
Looking for a reprint of this article?
From high-res PDFs to custom plaques, order your copy today!




